By: Bernadette Lou Caluya, MD, DPDS
What is Shingles?
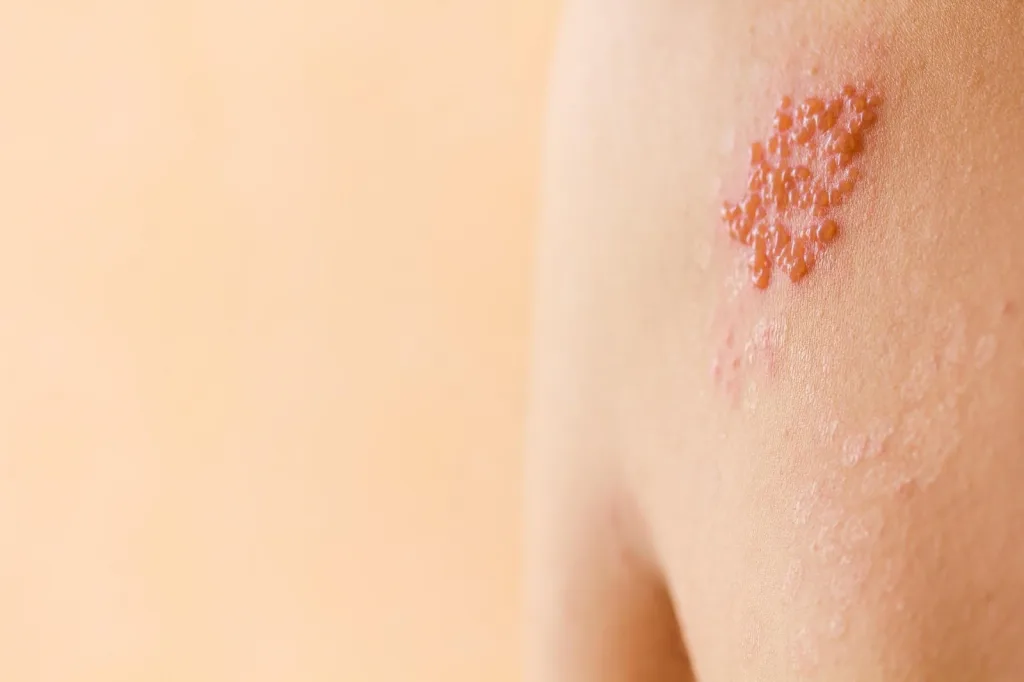
Shingles is a skin condition characterized by grouped vesicles with a reddish base in a band-like distribution usually affecting just one side of the body.
What causes Shingles?
Shingles is caused by Herpes Zoster Virus (HSV), which is also the virus that causes chickenpox. Shingles occur in people who already had chickenpox at one point in their lives. When a patient is healed from chickenpox clinically, HSV goes into a “resting” mode or latent mode in the neurons. When the same patient’s immune system experiences a decline, this virus can reactivate and can cause the expected skin lesions on the areas of the body supplied by the affected neurons.
Who gets Shingles?
Anyone can get Shingles but the following groups of people have increased risk in acquiring the disease
– elderly
– immunocompromised individuals (organ transplant patients, cancer patients)
– patients with immune-mediated conditions (systemic lupus erythematosus, rheumatoid arthritis etc.)
– patients undergoing chemotherapy, immunomodulators and corticosteroids
– HIV patients
What are the physical findings?
The lesions usually start as red patches on the affected body part in a unilateral distribution. After 12 to 24 hrs, grouped vesicles form on top of the patches. On the 3rd day, these vesicles can be filled with pus. In 7 to 10 days, brown crusts can form on top of the lesions. These crusts can persists for 2 to 3 weeks
What are the other signs and symptoms?
- Pain- described as burning, deep-aching, tingling, stabbing or lancinating. It can occur as early as 1 to 3 days prior to the appearance of the skin lesions
- Paresthesia- “pins and needles” on the affected areas
- Pruritus- can be apparent in the early stages of the disease until the crusts fall off
Is it infectious?
YES, Herpes Zoster Virus infection is infectious. A patient can transmit it to other people through direct contact with the vesicles until 7 days from the initial appearance of the skin lesions. It can also be airborne in some cases. The people who have exposure with patients with Shingles won’t develop Shingles, they will develop chickenpox.
It is important for patients to avoid exposure to pregnant mothers, elderly people, newborns and children.
Is it treatable?
YES, HZV infection is treatable.
– ORAL ANTI-VIRAL MEDICATIONS
It is important to seek consult with a dermatologist once the skin lesions are noted. Anti-viral medications are effective if given during the first 72 hours of the disease. It is proven that anti-viral therapy can decrease the duration and severity of the skin rash and associated pain. It also prevents the appearance of lesions to other parts of the body.
– TOPICAL TREATMENT OPTIONS
-can be beneficial during the acute phase to relieve pruritus and pain. It can also hasten the drying of
skin lesions
- Cool compress
- Calamine lotion
- Cornstarch
- TOPICAL CORTICOSTEROIDS should not be used
- anti-viral ointments or creams are not beneficial
What are the possible complications?
- Post –herpetic Neuralgia (PNH)- described as pain noted 1 to 6 months after the healing of the rash. Incidence and duration increases with age.
- Bacterial superinfection
- Scarring
- Pneumonitis, Hepatitis, Esophagitis
- Meningoencephalitis
- Deafness
- Eye complications
Is there a vaccine available?
Zostavax ® (live attenuated Oka/Merck strain VZV zoster vaccine) is available and recommended to adults >60 y/o of age for prevention of herpes zoster and its complications, especially post-herpetic neuralgia.