Stephanie Katalbas-Asi, MD, FPDS
What is diaper rash?
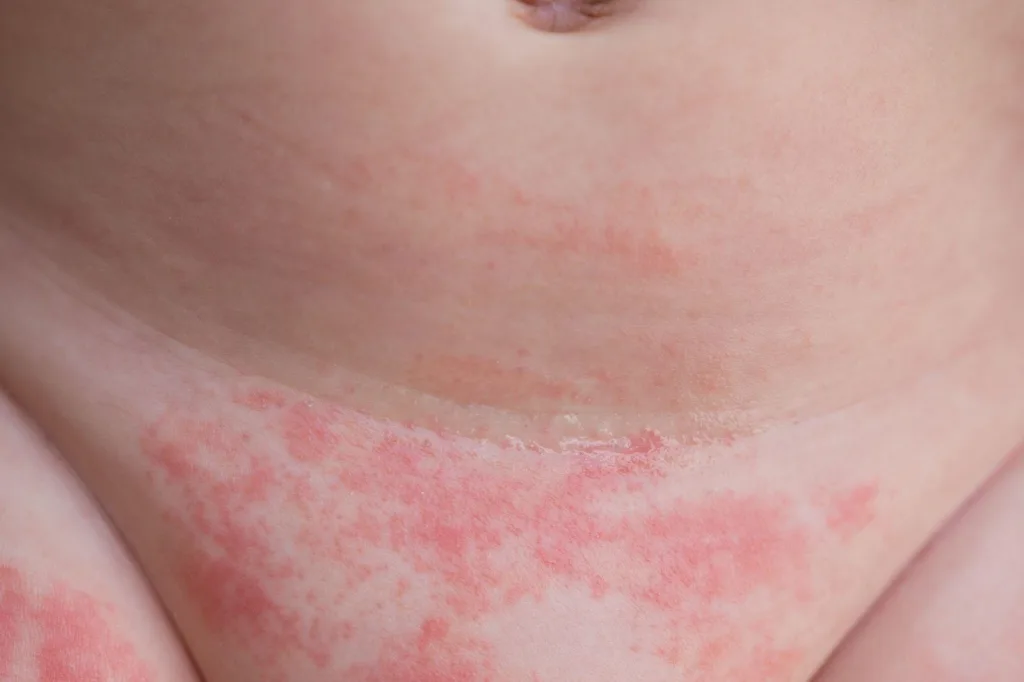
Diaper rash is a common form of reddish, inflamed skin on the areas covered by a diaper. This covers the genital area, buttocks, inner thighs, and sometimes the lower abdomen. This commonly affects babies, but it can also happen in adults who wear diapers.
In mild cases the skin can look pink, dry-looking skin, but in more severe cases it can resemble red, irritated, raw or burnt-looking skin with open wounds. It usually feels itchy or burning. Your child may seem more uncomfortable or irritable than usual, especially when changing diapers.
What causes diaper rash?
- Irritation from urine & stool. Prolonged exposure to urine or stool can irritate the skin. This is worsened by diarrhea and frequent bowel movements. It can also happen when introducing new foods, which alter the frequency of stools.
- Irritation or allergies to products like baby wipes, detergent or fabric conditioner, a new brand of disposable diapers, or certain ingredients of skin care products.
- Friction caused by tight-fitting diapers or clothing.
- Infection with yeast (fungi) and bacteria. These can start in the skin folds and spread to the surrounding skin. The diaper area is warm and moist, which makes it a good breeding ground for bacteria and yeast.
- ‘Sensitive skin’ conditions such as seborrheic dermatitis, atopic dermatitis (eczema), and psoriasis.
How is it treated?
The best thing to do is to keep the affected skin clean and dry as much as possible. Change diapers immediately after they are wet or soiled.
The exact treatment varies, depending on the exact cause for the diaper rash. This may include a mild steroid cream (e.g. hydrocortisone) and other antimicrobial creams. These medications should only be used under proper guidance from your doctor.
What can I do at home?
- Bathe the baby or adult daily using warm water with mild, fragrance-free soap.
- The affected areas may be air-dried to increase air exposure to the diaper region.
- After gently cleaning and drying the skin, certain products may be applied to protect the skin from moisture (e.g. zinc oxide paste, petroleum jelly). These may be removed by using a cotton ball with mineral oil, without scrubbing.
- Avoid air-tight plastic pants and diaper covers. In the meantime, bigger-than-usual diapers may be used until the rash improves.
- Avoid products that seem to trigger the diaper rash. Give the baby or adult as much diaper-free time as possible, to keep the skin dry and aid healing.
- In general, use only products designed for babies or sensitive skin. Avoid products containing baking soda, boric acid, camphor, phenol, benzocaine, or salicylates. These are irritating and can be toxic for babies.
How to prevent diaper rash?
- Keep the diaper area clean and dry. When possible, expose the skin to air as a gentle way to keep it dry.
- Change diapers promptly, as soon as they are wet or soiled.
- Rinse the affected areas with warm water after each diaper change. A moist washcloth or cotton balls may help, but use them gently. Avoid using wipes with alcohol or fragrance.
- Use properly-fitting diapers. Make sure they aren’t too tight, which will prevent airflow and cause chafing.
When should we see a doctor?
If the diaper rash doesn’t improve after 2-3 days with home treatment or shows any of the following changes, it’s best to consult a PDS certified Dermatologist for proper treatment.
- Swelling
- Small red pimple-like bumps outside the diaper area
- Blisters
- Yellow, fluid-filled bumps
- Honey-colored, crusty areas
- Bleeding
- Oozing with fluid or pus
- Fever
- Changes in behavior
Bibliography:
- Klunk, Christopher, et al. “An update on diaper dermatitis.” Clinics in Dermatology, vol. 32, 2014, pp. 477-487.
- Reider, Norbert, and Peter O. Fritsch. “Other Eczematous Eruptions.” Dermatology, 4 ed., vol. 1, Elsevier, 2018, pp. 228-241. 2 vols.
- Scheinfeld, Noah. “Diaper Dermatitis: A Review and Brief Survey of Eruptions of the Diaper Area.” Am J Clin Dermatol, vol. 6, no. 5, 2005, pp. 273-281.
Stamatas, Georgios N., and Neena K. Tierney. “Diaper Dermatitis: Etiology, Manifestations, Prevention, and Management.” Pediatric Dermatology, vol. 31, no. 1, 2014, pp. 1-7.